Insurance Verification Services
Insurance verification is the first — and one of the most critical — steps in the revenue cycle. At AverraBilling, we ensure that every patient’s coverage is verified before the service is rendered, reducing denials, delays, and lost revenue.
Get StartedVerify Faster. Bill Smarter.
Insurance verification is one of the most important — yet often overlooked — steps in the revenue cycle. At AverraBilling, we verify coverage, eligibility, and pre-authorizations upfront to reduce denials and accelerate reimbursement.

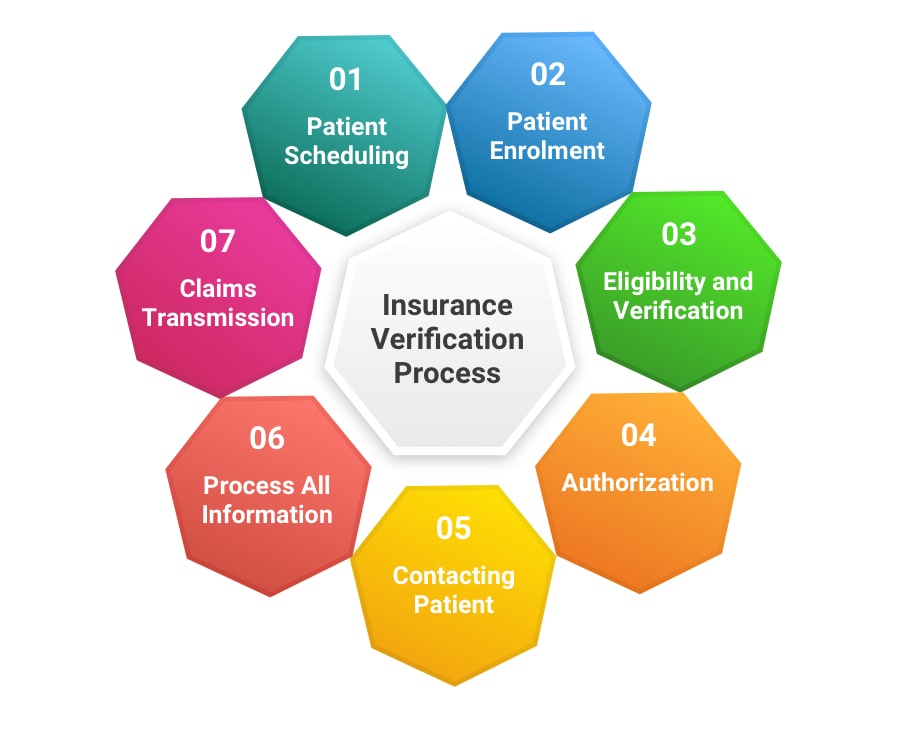
What We Verify
- Patient Eligibility: Real-time check for active coverage and policy status
- Plan Benefits: Verification of deductibles, co-pays, and limits
- Pre-Authorizations: Identify and secure required approvals
- Out-of-Network Status: Check eligibility for out-of-network services
- Secondary Insurance: Confirm COB and dual coverage
Benefits of Our Insurance Verification Services
- Fewer Claim Denials due to accurate, upfront data
- Faster Reimbursements from clean claim submission
- Improved Patient Experience with clear cost expectations
- Reduced Admin Burden on your in-house staff
- Increased Revenue Capture through fewer billing errors

Ready to Simplify Insurance Verification?
Let AverraBilling handle the details. With our expert team managing eligibility checks and coverage confirmations, you can focus on what matters most — delivering excellent patient care.

